Gonorrhea Can Be Passed From the Mother to Her Baby
| Gonorrhea | |
|---|---|
| Other names | Gonorrhoea, gonococcal infection, gonococcal urethritis, the clap |
 | |
| Gonococcal lesion on the skin | |
| Pronunciation | |
| Specialty | Infectious illness |
| Symptoms | None, burning with urination, vaginal discharge, belch from the penis, pelvic pain, testicular hurting[1] |
| Complications | Pelvic inflammatory disease, inflammation of the epididymis, septic arthritis, endocarditis[i] [ii] |
| Causes | Neisseria gonorrhoeae typically sexually transmitted[ane] |
| Diagnostic method | Testing the urine, urethra in males, or cervix in females[1] |
| Prevention | Condoms, having sex with only ane person who is uninfected, not having sex[1] [three] |
| Treatment | Ceftriaxone by injection and azithromycin by oral cavity[4] [v] |
| Frequency | 0.8% (women), 0.6% (men)[6] |
Gonorrhea, colloquially known as the clap, is a sexually transmitted infection (STI) acquired by the bacterium Neisseria gonorrhoeae.[1] Infection may involve the genitals, mouth, or rectum.[7] Infected men may experience pain or called-for with urination, discharge from the penis, or testicular pain.[1] Infected women may experience called-for with urination, vaginal belch, vaginal bleeding betwixt periods, or pelvic pain.[1] Complications in women include pelvic inflammatory disease and in men include inflammation of the epididymis.[1] Many of those infected, still, have no symptoms.[i] If untreated, gonorrhea tin spread to joints or center valves.[i] [2]
Gonorrhea is spread through sexual contact with an infected person.[one] This includes oral, anal, and vaginal sex activity.[1] It can also spread from a mother to a child during birth.[1] Diagnosis is by testing the urine, urethra in males, or cervix in females.[i] Testing all women who are sexually agile and less than 25 years of age each yr as well as those with new sexual partners is recommended;[3] the same recommendation applies in men who have sex with men (MSM).[three]
Gonorrhea can be prevented with the use of condoms, having sex with simply one person who is uninfected, and by not having sex activity.[one] [three] Treatment is usually with ceftriaxone by injection and azithromycin by mouth.[four] [five] Resistance has developed to many previously used antibiotics and college doses of ceftriaxone are occasionally required.[4] [5] Retesting is recommended three months later treatment.[iii] Sexual partners from the terminal ii months should also be treated.[i]
Gonorrhea affects nearly 0.8% of women and 0.vi% of men.[six] An estimated 33 to 106 meg new cases occur each year, out of the 498 one thousand thousand new cases of curable STI – which besides includes syphilis, chlamydia, and trichomoniasis.[8] [9] Infections in women most commonly occur when they are young adults.[3] In 2015, it caused about 700 deaths.[10] Descriptions of the disease date dorsum to before the Common Era within the Old Testament.[2] The electric current proper name was first used by the Greek physician Galen before 200 CE who referred to it as "an unwanted discharge of semen".[2]
Signs and symptoms
Gonorrhea infections of mucosal membranes can cause swelling, itching, hurting, and the germination of pus.[xi] The time from exposure to symptoms is usually betwixt two and fourteen days, with nearly symptoms appearing between 4 and six days after infection, if they appear at all. Both men and women with infections of the throat may feel a sore pharynx, though such infection does not produce symptoms in 90% of cases.[12] [thirteen] Other symptoms may include swollen lymph nodes around the neck.[11] Either sex can become infected in the eyes or rectum if these tissues are exposed to the bacterium.[ citation needed ]
Women
One-half of women with gonorrhea are asymptomatic but the other half feel vaginal discharge, lower abdominal pain, or hurting with sexual intercourse associated with inflammation of the uterine cervix.[fourteen] [15] [16] Common medical complications of untreated gonorrhea in women include pelvic inflammatory disease which can cause scars to the fallopian tubes and result in later ectopic pregnancy amongst those women who become meaning.[17]
Men
Most infected men with symptoms take inflammation of the penile urethra associated with a called-for sensation during urination and discharge from the penis.[15] In men, discharge with or without called-for occurs in one-half of all cases and is the most common symptom of the infection.[18] This pain is caused by a narrowing and stiffening of the urethral lumen.[19] The most mutual medical complexity of gonorrhea in men is inflammation of the epididymis.[17] Gonorrhea is likewise associated with increased risk of prostate cancer.[twenty]
Infants
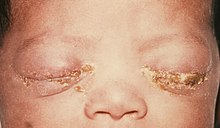
An infant with gonorrhea of the eyes
If not treated, gonococcal ophthalmia neonatorum volition develop in 28% of infants born to women with gonorrhea.[21]
Spread
If left untreated, gonorrhea tin spread from the original site of infection and infect and impairment the joints, skin, and other organs. Indications of this can include fever, skin rashes, sores, and joint pain and swelling.[17] In avant-garde cases, gonorrhea may cause a general feeling of tiredness similar to other infections.[eighteen] Information technology is also possible for an individual to accept an allergic reaction to the bacteria, in which case any actualization symptoms will be greatly intensified.[18] Very rarely information technology may settle in the heart, causing endocarditis, or in the spinal column, causing meningitis. Both are more likely amid individuals with suppressed immune systems, however.[13]
Cause

Gonorrhea is caused by the bacterium Neisseria gonorrhoeae.[15] Previous infection does not confer immunity – a person who has been infected can go infected again by exposure to someone who is infected. Infected persons may exist able to infect others repeatedly without having any signs or symptoms of their own.[ commendation needed ]
Spread
The infection is unremarkably spread from one person to some other through vaginal, oral, or anal sex activity.[xv] [22] Men have a twenty% risk of getting the infection from a single act of vaginal intercourse with an infected woman. The take a chance for men that have sex with men (MSM) is higher.[23] Insertive MSM may get a penile infection from anal intercourse, while receptive MSM may become anorectal gonorrhea.[24] Women accept a threescore–eighty% run a risk of getting the infection from a single act of vaginal intercourse with an infected man.[25]
A mother may transmit gonorrhea to her newborn during childbirth; when affecting the baby'due south eyes, it is referred to equally ophthalmia neonatorum.[15] Information technology may be able to spread through the objects contaminated with torso fluid from an infected person.[26] The bacteria typically does not survive long outside the body, typically dying within minutes to hours.[27]
Diagnosis
Traditionally, gonorrhea was diagnosed with Gram stain and culture; however, newer polymerase chain reaction (PCR)-based testing methods are condign more than common.[xvi] [28] In those failing initial handling, culture should be done to decide sensitivity to antibiotics.[29]
Tests that use PCR (aka nucleic acrid amplification) to identify genes unique to N. gonorrhoeae are recommended for screening and diagnosis of gonorrhea infection. These PCR-based tests crave a sample of urine, urethral swabs, or cervical/vaginal swabs. Civilisation (growing colonies of bacteria in order to isolate and identify them) and Gram-stain (staining of bacterial prison cell walls to reveal morphology) tin can as well exist used to detect the presence of Northward. gonorrhoeae in all specimen types except urine.[xxx] [31]
If Gram-negative, oxidase-positive diplococci are visualized on straight Gram stain of urethral pus (male person genital infection), no further testing is needed to found the diagnosis of gonorrhea infection.[32] [33] However, in the case of female infection direct Gram stain of cervical swabs is non useful because the Northward. gonorrhoeae organisms are less concentrated in these samples. The chances of false positives are increased equally Gram-negative diplococci native to the normal vaginal flora cannot be distinguished from N. gonorrhoeae. Thus, cervical swabs must be cultured under the atmospheric condition described above. If oxidase positive, Gram-negative diplococci are isolated from a culture of a cervical/vaginal swab specimen, so the diagnosis is made. Civilisation is peculiarly useful for diagnosis of infections of the throat, rectum, eyes, blood, or joints—areas where PCR-based tests are not well established in all labs.[33] [34] Civilization is also useful for antimicrobial sensitivity testing, handling failure, and epidemiological purposes (outbreaks, surveillance).[33]
In patients who may have disseminated gonococcal infection (DGI), all possible mucosal sites should be cultured (east.yard., throat, cervix, urethra, rectum).[34] Three sets of claret cultures should as well be obtained.[35] Synovial fluid should exist collected in cases of septic arthritis.[34]
All people testing positive for gonorrhea should be tested for other sexually transmitted diseases such as chlamydia, syphilis, and human immunodeficiency virus.[29] Studies take found co-infection with chlamydia ranging from 46 to 54% in immature people with gonorrhea.[36] [37] Among persons in the United States between xiv and 39 years of age, 46% of people with gonorrheal infection also have chlamydial infection.[38] For this reason, gonorrhea and chlamydia testing are oft combined.[thirty] [39] [40] People diagnosed with gonorrhea infection accept a fivefold increase take chances of HIV transmission.[41] Additionally, infected persons who are HIV positive are more likely to shed and transmit HIV to uninfected partners during an episode of gonorrhea.[42]
Screening
The Usa Preventive Services Task Force (USPSTF) recommends screening for gonorrhea in women at increased hazard of infection, which includes all sexually active women younger than 25 years. Extragenital gonorrhea and chlamydia are highest in men who have sex with men (MSM).[43] Additionally, the USPSTF also recommends routine screening in people who have previously tested positive for gonorrhea or have multiple sexual partners and individuals who utilise condoms inconsistently, provide sexual favors for coin, or take sexual practice while nether the influence of alcohol or drugs.[14]
Screening for gonorrhea in women who are (or intend to get) pregnant, and who are constitute to be at high risk for sexually transmitted diseases, is recommended equally function of prenatal care in the United States.[44]
Prevention
As with about sexually transmitted diseases, the chance of infection tin exist reduced significantly past the correct employ of condoms, non having sex, or can be removed almost entirely by limiting sexual activities to a mutually monogamous relationship with an uninfected person.[45] [46]
Those previously infected are encouraged to return for follow up care to brand certain that the infection has been eliminated. In improver to the use of phone contact, the apply of electronic mail and text messaging have been found to improve the re-testing for infection.[47]
Newborn babies coming through the nascence canal are given erythromycin ointment in the optics to forbid blindness from infection. The underlying gonorrhea should be treated; if this is done then usually a good prognosis will follow.[48]
Treatment
Antibiotics

Penicillin entered mass production in 1944 and revolutionized the treatment of several venereal diseases.
Antibiotics are used to treat gonorrhea infections. As of 2016, both ceftriaxone past injection and azithromycin by mouth are nigh effective.[4] [49] [fifty] [51] All the same, due to increasing rates of antibiotic resistance, local susceptibility patterns must be taken into business relationship when deciding on treatment.[29] [52]
Adults may take eyes infected with gonorrhoea and require proper personal hygiene and medications.[48] Addition of topical antibiotics take not been shown to improve cure rates compared to oral antibiotics alone in handling of middle infected gonorrhea.[53] For newborns, erythromycin ointment is recommended as a preventative measure for gonococcal infant conjunctivitis.[54]
Infections of the throat tin exist especially problematic, as antibiotics take difficulty becoming sufficiently concentrated there to destroy the bacteria. This is amplified by the fact that pharyngeal gonorrhoea is mostly asymptomatic, and gonococci and commensal Neisseria species can coexist for long time periods in the throat and share anti-microbial resistance genes. Appropriately, an enhanced focus on early detection (i.e., screening of high-risk populations, such as men who accept sexual activity with men, PCR testing should be considered) and appropriate treatment of pharyngeal gonorrhoea is important.[4]
Sexual partners
Information technology is recommended that sexual partners exist tested and potentially treated.[29] One pick for treating sexual partners of people infected is patient-delivered partner therapy (PDPT), which involves providing prescriptions or medications to the person to have to his/her partner without the wellness intendance provider's first examining him/her.[55]
The United states of america' Centers for Disease Control and Prevention (CDC) currently recommend that individuals who accept been diagnosed and treated for gonorrhea avert sexual contact with others until at least one week by the final twenty-four hour period of treatment in order to prevent the spread of the bacterium.[56]
Antibody resistance
Many antibiotics that were once effective including penicillin, tetracycline, and fluoroquinolones are no longer recommended because of high rates of resistance.[29] Resistance to cefixime has reached a level such that information technology is no longer recommended as a first-line agent in the Usa, and if it is used a person should be tested once again afterwards a calendar week to determine whether the infection still persists.[49] Public wellness officials are concerned that an emerging design of resistance may predict a global epidemic.[57] The UK's Health Protection Agency reported that 2011 saw a slight driblet in gonorrhea antibiotic resistance, the commencement in five years.[58] In 2016, the WHO published new guidelines for treatment, stating "There is an urgent need to update treatment recommendations for gonococcal infections to respond to changing antimicrobial resistance (AMR) patterns of N. gonorrhoeae. High-level resistance to previously recommended quinolones is widespread and decreased susceptibility to the extended-spectrum (3rd-generation) cephalosporins, another recommended kickoff-line treatment in the 2003 guidelines, is increasing and several countries accept reported treatment failures."[59]
Prognosis

Inability-adjusted life year for gonorrhea per 100,000 inhabitants
| no data <13 xiii–26 26–39 39–52 52–65 65–78 | 78–91 91–104 104–117 117–130 130–143 >143 |
Gonorrhea if left untreated may last for weeks or months with higher risks of complications.[xv] One of the complications of gonorrhea is systemic dissemination resulting in pare pustules or petechia, septic arthritis, meningitis, or endocarditis.[xv] This occurs in between 0.6 and iii% of infected women and 0.4 and 0.7% of infected men.[15]
In men, inflammation of the epididymis, prostate gland, and urethra tin can result from untreated gonorrhea.[60] In women, the nigh common result of untreated gonorrhea is pelvic inflammatory disease. Other complications include inflammation of the tissue surrounding the liver,[60] a rare complication associated with Fitz-Hugh–Curtis syndrome; septic arthritis in the fingers, wrists, toes, and ankles; septic abortion; chorioamnionitis during pregnancy; neonatal or adult blindness from conjunctivitis; and infertility. Men who have had a gonorrhea infection have an increased risk of getting prostate cancer.[20]
Epidemiology

Gonorrhea rates, Us, 1941–2007
About 88 million cases of gonorrhea occur each year, out of the 448 million new cases of curable STI each year – that too includes syphilis, chlamydia and trichomoniasis.[nine] The prevalence was highest in the African region, the Americas, and Western Pacific, and everyman in Europe.[61] In 2013, information technology caused about iii,200 deaths, upwards from ii,300 in 1990.[62]
In the United Kingdom, 196 per 100,000 males 20 to 24 years erstwhile and 133 per 100,000 females sixteen to nineteen years onetime were diagnosed in 2005.[15] In 2013, the CDC estimated that more than 820,000 people in the The states get a new gonorrheal infection each year. Fewer than half of these infections are reported to CDC. In 2011, 321,849 cases of gonorrhea were reported to the CDC. Subsequently the implementation of a national gonorrhea command program in the mid-1970s, the national gonorrhea charge per unit declined from 1975 to 1997. After a small increment in 1998, the gonorrhea rate has decreased slightly since 1999. In 2004, the rate of reported gonorrheal infections was 113. 5 per 100,000 persons.[63]
In the US, it is the second-virtually-common bacterial sexually transmitted infections; chlamydia remains first.[64] [65] Co-ordinate to the CDC African Americans are nearly affected by gonorrhea, accounting for 69% of all gonorrhea cases in 2010.[66]
The World Wellness Organization warned in 2017 of the spread of untreatable strains of gonorrhea, following analysis of at to the lowest degree iii cases in Japan, France and Spain, which survived all antibody handling.[67]
History

Some scholars translate the biblical terms zav (for a male) and zavah (for a female person) as gonorrhea.[68]
Information technology has been suggested that mercury was used as a treatment for gonorrhea. Surgeons' tools on board the recovered English language warship the Mary Rose included a syringe that, according to some, was used to inject the mercury via the urinary meatus into crewmen suffering from gonorrhea. The name "the clap", in reference to the illness, is recorded as early every bit the sixteenth century, referring to a medieval red-light district in Paris, Les Clapiers. Translating to "The rabbit holes", it was and then named for the small huts in which prostitutes worked.[69] [70]
In 1854, Dr. Wilhelm Gollmann addressed gonorrhea in his volume, Homeopathic Guide to all Diseases Urinary and Sexual Organs. He noted that the disease was common in prostitutes and homosexuals in big cities. Gollmann recommended the following as cures: aconite to cure "shooting pains with soreness and inflammation;" mercury "for stitching pain with purulent belch;" nux vomica and sulphur "when the symptoms are complicated with hemorrhoids and stricture of the rectum. Other remedies include argentum, aurum (gold), belladonna, calcarea, ignatia, phosphorus, and sepia.[24]
Silver nitrate was 1 of the widely used drugs in the 19th century. However, it became replaced by Protargol. Arthur Eichengrün invented this type of colloidal silver, which was marketed past Bayer from 1897 onward. The silver-based treatment was used until the first antibiotics came into apply in the 1940s.[71] [72]
The verbal time of onset of gonorrhea every bit prevalent illness or epidemic cannot be accurately determined from the historical record. I of the starting time reliable notations occurs in the Acts of the (English language) Parliament. In 1161, this body passed a law to reduce the spread of "... the perilous infirmity of burning".[73] The symptoms described are consistent with, but non diagnostic of, gonorrhea. A similar prescript was passed by Louis IX in French republic in 1256, replacing regulation with banishment.[74] Like symptoms were noted at the siege of Acre by Crusaders.
Coincidental to, or dependent on, the appearance of a gonorrhea epidemic, several changes occurred in European medieval society. Cities hired public health doctors to care for afflicted patients without right of refusal. Pope Boniface rescinded the requirement that physicians complete studies for the lower orders of the Catholic priesthood.[75]
Medieval public health physicians in the employ of their cities were required to care for prostitutes infected with the "burning", too as lepers and other epidemic victims.[76] After Pope Boniface completely secularized the practice of medicine, physicians were more willing to treat a sexually transmitted illness.[75]
Research
A vaccine for gonorrhea has been developed that is effective in mice.[77] It volition non be available for human use until further studies have demonstrated that it is both safe and effective in the human being population. Evolution of a vaccine has been complicated by the ongoing evolution of resistant strains and antigenic variation (the ability of N. gonorrhoeae to disguise itself with different surface markers to evade the allowed system).[52]
As N. gonorrhoeae is closely related to N. meningitidis and they accept 80–90% homology in their genetic sequences some cross-protection by meningococcal vaccines is plausible. A written report published in 2017 showed that MeNZB group B meningococcal vaccine provided a fractional protection confronting gonorrhea.[78] The vaccine efficiency was calculated to be 31%.[79]
References
- ^ a b c d east f yard h i j k l m n o p q "Gonorrhea – CDC Fact Sheet (Detailed Version)". CDC. 17 November 2015. Archived from the original on 2 September 2016. Retrieved 27 Baronial 2016.
- ^ a b c d Morgan, MK; Decker, CF (August 2016). "Gonorrhea". Affliction-a-Calendar month. 62 (8): 260–8. doi:10.1016/j.disamonth.2016.03.009. PMID 27107780.
- ^ a b c d e f Workowski, KA; Bolan, GA (5 June 2015). "Sexually transmitted diseases treatment guidelines, 2015". MMWR. Recommendations and Reports. 64 (RR-03): 1–137. PMC5885289. PMID 26042815.
- ^ a b c d e "Antibiotic-Resistant Gonorrhea Bones Information". CDC. xiii June 2016. Archived from the original on 8 September 2016. Retrieved 27 August 2016.
- ^ a b c Unemo, M (21 Baronial 2015). "Electric current and future antimicrobial treatment of gonorrhoea – the rapidly evolving Neisseria gonorrhoeae continues to challenge". BMC Infectious Diseases. 15: 364. doi:ten.1186/s12879-015-1029-2. PMC4546108. PMID 26293005.
- ^ a b Newman, Lori; Rowley, Jane; Vander Hoorn, Stephen; Wijesooriya, Nalinka Saman; Unemo, Magnus; Low, Nicola; Stevens, Gretchen; Gottlieb, Sami; Kiarie, James; Temmerman, Marleen; Meng, Zhefeng (8 December 2015). "Global Estimates of the Prevalence and Incidence of Four Curable Sexually Transmitted Infections in 2012 Based on Systematic Review and Global Reporting". PLOS ONE. 10 (12): e0143304. Bibcode:2015PLoSO..1043304N. doi:ten.1371/journal.pone.0143304. PMC4672879. PMID 26646541.
- ^ Leslie Delong; Nancy Burkhart (27 Nov 2017). General and Oral Pathology for the Dental Hygienist. Wolters Kluwer Wellness. p. 787. ISBN978-1-4963-5453-2.
- ^ Global Burden of Disease Study 2013, Collaborators (22 Baronial 2015). "Global, regional, and national incidence, prevalence, and years lived with inability for 301 astute and chronic diseases and injuries in 188 countries, 1990–2013: a systematic analysis for the Global Brunt of Disease Written report 2013". Lancet. 386 (9995): 743–800. doi:ten.1016/s0140-6736(15)60692-4. PMC4561509. PMID 26063472.
- ^ a b Emergence of multi-drug resistant Neisseria gonorrhoeae (PDF) (Report). World Health Organisation. 2012. p. 2. Archived from the original (PDF) on 12 September 2014.
- ^ GBD 2015 Mortality and Causes of Expiry, Collaborators. (8 Oct 2016). "Global, regional, and national life expectancy, all-cause mortality, and cause-specific mortality for 249 causes of death, 1980–2015: a systematic analysis for the Global Brunt of Disease Study 2015". Lancet. 388 (10053): 1459–1544. doi:ten.1016/s0140-6736(sixteen)31012-1. PMC5388903. PMID 27733281.
- ^ a b "Gonorrhea - Symptoms and causes". Mayo Clinic . Retrieved 6 August 2019.
- ^ Zakher, Bernadette; Cantor MD, Amy G.; Daeges, Monica; Nelson Md, Heidi (16 December 2014). "Review: Screening for Gonorrhea and Chlamydia: A Systematic Review for the U.S. Prevententive Services Job Force". Annals of Internal Medicine. 161 (12): 884–894. CiteSeerXx.1.i.691.6232. doi:10.7326/M14-1022. PMID 25244000. S2CID 207538182.
- ^ a b Marr, Lisa (2007) [1998]. Sexually Transmitted Diseases: A Md Tells You What You Need to Know (Second ed.). Baltimore, Maryland: Johns Hopkins University. ISBN978-0-8018-8658-iv.
- ^ a b Smith, 50; Angarone, MP (November 2015). "Sexually Transmitted Infections". The Urologic Clinics of North America. 42 (4): 507–eighteen. CiteSeerX10.1.1.590.3827. doi:x.1016/j.ucl.2015.06.004. PMID 26475947.
- ^ a b c d e f 1000 h i Moran JS (2007). "Gonorrhoea". Clin Evid (Online). 2007. PMC2943790. PMID 19454057.
- ^ a b Ljubin-Sternak, Suncanica; Mestrovic, Tomislav (2014). "Review: Chlamydia trachonmatis and Genital Mycoplasmias: Pathogens with an Impact on Human Reproductive Wellness". Periodical of Pathogens. 2014 (183167): vii. doi:10.1155/2014/183167. PMC4295611. PMID 25614838.
- ^ a b c "What Complications Can Gonorrhea Cause?". WebMD. 2019.
- ^ a b c Brian R. Shmaefsky (1 January 2009). Gonorrhea. Infobase. p. 52. ISBN978-one-4381-0142-two.
- ^ Liang Cheng; David One thousand. Bostwick (24 January 2014). Urologic Surgical Pathology Eastward-Volume. Elsevier Health Sciences. p. 863. ISBN978-0-323-08619-6.
- ^ a b Caini, Saverio; Gandini, Sara; Dudas, Maria; Bremer, Viviane; Severi, Ettore; Gherasim, Alin (2014). "Sexually transmitted infections and prostate cancer run a risk: A systematic review and meta-analysis". Cancer Epidemiology. 38 (4): 329–338. doi:10.1016/j.canep.2014.06.002. PMID 24986642.
- ^ "Prophylaxis for Gonococcal and Chlamydial Ophthalmia Neonatorum in the Canadian Guide to Clinical Preventative Health Care" (PDF). Public Wellness Agency of Canada. Archived from the original (PDF) on 10 March 2010.
- ^ Trebach, Joshua D.; Chaulk, C. Patrick; Page, Kathleen R.; Tuddenham, Susan; Ghanem, Khalil G. (2015). "Neisseria gonorrhoeae and Chlamydia trachomatis Among Women Reporting Extragenital Exposures". Sexually Transmitted Diseases. 42 (5): 233–239. doi:10.1097/OLQ.0000000000000248. ISSN 0148-5717. PMC4672628. PMID 25868133.
- ^ Howard Chocolate-brown Health Eye: STI Annual Study, 2009
- ^ a b Gollmann, Wilhelm (1854). Homeopathic Guide to all Diseases Urinary and Sexual Organ. Charles Julius Hempel. Rademacher & Sheek.
- ^ National Institute of Allergy and Infectious Diseases; National Institutes of Wellness, Department of Health and Human Services (xx July 2001). "Workshop Summary: Scientific Show on Safe Effectiveness for Sexually Transmitted Illness (STD) Prevention". Hyatt Dulles Airport, Herndon, Virginia. pp14
- ^ Goodyear-Smith, F (November 2007). "What is the evidence for non-sexual transmission of gonorrhoea in children after the neonatal period? A systematic review". Journal of Forensic and Legal Medicine. xiv (eight): 489–502. doi:x.1016/j.jflm.2007.04.001. PMID 17961874.
- ^ Brian R. Shmaefsky (1 January 2009). Gonorrhea. Infobase. p. 48. ISBN978-1-4381-0142-ii.
- ^ Barry PM, Klausner JD (March 2009). "The use of cephalosporins for gonorrhea: The impending problem of resistance". Skillful Opin Pharmacother. 10 (four): 555–77. doi:ten.1517/14656560902731993. PMC2657229. PMID 19284360.
- ^ a b c d e Deguchi T, Nakane K, Yasuda One thousand, Maeda South (September 2010). "Emergence and spread of drug resistant Neisseria gonorrhoeae". J. Urol. 184 (3): 851–viii, quiz 1235. doi:ten.1016/j.juro.2010.04.078. PMID 20643433.
- ^ a b "Final Recommendation Statement: Chlamydia and Gonorrhea: Screening – US Preventive Services Job Force". uspreventiveservicestaskforce.org . Retrieved 7 Dec 2017.
- ^ "Gonococcal Infections – 2015 STD Handling Guidelines". cdc.gov . Retrieved seven December 2017.
- ^ Levinson, Warren (1 July 2014). Review of medical microbiology and immunology (Thirteenth ed.). New York. ISBN9780071818117. OCLC 871305336.
- ^ a b c Ng, Lai-King; Martin, Irene E (2005). "The laboratory diagnosis of Neisseria gonorrhoeae". The Canadian Journal of Infectious Diseases & Medical Microbiology. sixteen (1): xv–25. doi:10.1155/2005/323082. ISSN 1712-9532. PMC2095009. PMID 18159523.
- ^ a b c https://www.cdc.gov/std/tg2015/clinical.htm section on prevention methods
- ^ Gonorrhea~overview at eMedicine
- ^ Kahn, Richard H.; Mosure, Debra J.; Bare, Susan; Kent, Charlotte Chiliad.; Chow, Joan M.; Boudov, Melina R.; Brock, Jeffrey; Tulloch, Scott; Jail STD Prevalence Monitoring Project (April 2005). "Chlamydia trachomatis and Neisseria gonorrhoeae prevalence and coinfection in adolescents entering selected US juvenile detention centers, 1997–2002". Sexually Transmitted Diseases. 32 (iv): 255–259. doi:10.1097/01.olq.0000158496.00315.04. ISSN 0148-5717. PMID 15788927. S2CID 20864079.
- ^ Dicker, Linda Due west.; Mosure, Debra J.; Berman, Stuart M.; Levine, William C. (May 2003). "Gonorrhea prevalence and coinfection with chlamydia in women in the United States, 2000". Sexually Transmitted Diseases. thirty (5): 472–476. doi:10.1097/00007435-200305000-00016. ISSN 0148-5717. PMID 12916141. S2CID 39361152.
- ^ Datta, SD; Sternberg, M; Johnson, RE; Berman, S; Papp, JR; McQuillan, G; Weinstock, H (17 July 2007). "Gonorrhea and chlamydia in the United States among persons 14 to 39 years of historic period, 1999 to 2002". Annals of Internal Medicine. 147 (2): 89–96. doi:ten.7326/0003-4819-147-2-200707170-00007. PMID 17638719.
- ^ "Gonococcal Infections - 2015 STD Treatment Guidelines". 4 January 2018.
- ^ Ryan, KJ; Ray, CG, eds. (2004). Sherris Medical Microbiology (4th ed.). McGraw Hill. ISBN978-0-8385-8529-0. [ page needed ]
- ^ Department of Reproductive Health and Research (2011). "Emergence of multi-drug resistant Neisseria gonorrhoeae – Threat of global rise in untreatable sexually transmitted infections" (PDF). FactSheet WHO/RHR/11.14. World Health Organisation.
- ^ "Gonorrhea – STD information from CDC". cdc.gov. 6 October 2017. Retrieved five December 2017.
- ^ Meyers D; Wolff T; Gregory K; et al. (March 2008). "USPSTF recommendations for STI screening". Am Fam Physician. 77 (half dozen): 819–24. PMID 18386598.
- ^ Wellness Care Guideline: Routine Prenatal Care. Fourteenth Edition. Archived 5 July 2008 at the Wayback Car Past the Found for Clinical Systems Comeback July 2010.
- ^ department: Prevention Archived xx July 2013 at the Wayback Machine
- ^ section: How tin can gonorrhea be prevented? Archived 16 December 2016 at the Wayback Auto
- ^ Desai, Monica; Woodhall, Sarah C; Nardone, Anthony; Burns, Fiona; Mercey, Danielle; Gilson, Richard (2015). "Active recall to increase HIV and STI testing: a systematic review". Sexually Transmitted Infections. 91 (5): sextrans–2014–051930. doi:10.1136/sextrans-2014-051930. ISSN 1368-4973. PMID 25759476.
- ^ a b Sadowska-Przytocka, A; Czarnecka-Operacz, Thou; Jenerowicz, D; Grzybowski, A (2016). "Ocular manifestations of infectious pare diseases". Clinics in Dermatology. 34 (ii): 124–viii. doi:x.1016/j.clindermatol.2015.11.010. PMID 26903179.
- ^ a b Centers for Disease Control and Prevention, (CDC) (ten Baronial 2012). "Update to CDC'southward Sexually Transmitted Diseases Treatment Guidelines, 2010: Oral Cephalosporins No Longer a Recommended Treatment for Gonococcal Infections". MMWR. Morbidity and Mortality Weekly Written report. 61 (31): 590–4. PMID 22874837.
- ^ "Antibiotic-resistant gonorrhoea on the ascension, new drugs needed". Globe Health Organisation. 7 July 2017. Archived from the original on 9 July 2017. Retrieved 10 July 2017.
- ^ Sánchez-Busó, Leonor; Golparian, Daniel; Corander, Jukka; Grad, Yonatan H.; Ohnishi, Makoto; Flemming, Rebecca; Parkhill, Julian; Bentley, Stephen D.; Unemo, Magnus (29 July 2019). "The impact of antimicrobials on gonococcal evolution". Nature Microbiology. four (11): 1941–1950. doi:10.1038/s41564-019-0501-y. ISSN 2058-5276. PMC6817357. PMID 31358980.
- ^ a b Baarda, Benjamin I.; Sikora, Aleksandra Due east. (2015). "Proteomics of Neisseria gonorrhoeae: the treasure hunt for countermeasures against an old affliction". Frontiers in Microbiology. half dozen: 1190. doi:10.3389/fmicb.2015.01190. ISSN 1664-302X. PMC4620152. PMID 26579097; Access provided by the University of Pittsburgh.
{{cite journal}}: CS1 maint: postscript (link) - ^ Epling, John (20 February 2012). "Bacterial conjunctivitis". BMJ Clinical Show. 2012. ISSN 1752-8526. PMC3635545. PMID 22348418.
- ^ US Preventive Services Job Force; Curry, Susan J.; Krist, Alex H.; Owens, Douglas One thousand.; Barry, Michael J.; Caughey, Aaron B.; Davidson, Karina Westward.; Doubeni, Chyke A.; Epling, John W. (29 January 2019). "Ocular Prophylaxis for Gonococcal Ophthalmia Neonatorum: US Preventive Services Task Forcefulness Reaffirmation Recommendation Statement". JAMA. 321 (4): 394–398. doi:10.1001/jama.2018.21367. ISSN 1538-3598. PMID 30694327.
- ^ "Expedited partner therapy in the direction of sexually transmitted diseases" Archived 2 November 2009 at the Wayback Auto. February 2006. Centers for Illness Control and Prevention (CDC).
- ^ CDC (14 July 2014). "Gonorrhea – CDC Fact Sheet". Archived from the original on xvi December 2016. Retrieved 17 Oct 2014.
- ^ Groopman, Jerome (1 October 2012). "Sex and the Superbug". The New Yorker. Vol. LXXXVIII, no. 30. pp. 26–31. Archived from the original on 9 October 2012. Retrieved 13 October 2012.
...public-wellness experts [see]...the emergence of a strain of gonorrhea that is resistant to the final drug bachelor against it, and the harbinger of a sexually transmitted global epidemic.
- ^ "Gonorrhoea treatment resistance risk falls but new diagnoses rise". Health Protection Agency. 12 September 2012. Archived from the original on 14 July 2014.
- ^ "WHO guidelines for the handling of Neisseria gonorrhoeae". World Health Arrangement. 2016. Retrieved 24 September 2020.
- ^ a b Kumar, Vinay; Abbas, Abul One thousand.; Fausto, Nelson; & Mitchell, Richard North. (2007). Robbins Basic Pathology (8th ed.). Saunders Elsevier. pp. 705–706 ISBN 978-1-4160-2973-ane
- ^ Kirkcaldy, R. D.; Weston, E.; Segurado, A. C.; Hughes, One thousand. (September 2019). "Epidemiology of Gonorrhea: A Global Perspective". Sex activity Health. United States National Library of Medicine. 16 (five): 401–411. doi:10.1071/SH19061. PMC7064409. PMID 31505159.
- ^ GBD 2013 Mortality and Causes of Expiry, Collaborators (x Jan 2015). "Global, regional, and national historic period-sex specific all-cause and crusade-specific mortality for 240 causes of death, 1990–2013: a systematic analysis for the Global Burden of Disease Study 2013". Lancet. 385 (9963): 117–71. doi:10.1016/s0140-6736(xiv)61682-ii. PMC4340604. PMID 25530442.
- ^ "Gonorrhea – CDC Fact Sheet". CDC. 29 May 2012. Archived from the original on 16 December 2016. Retrieved 20 December 2013.
- ^ "CDC – STD Surveillance – Gonorrhea". Archived from the original on half-dozen March 2008. Retrieved 21 August 2008.
- ^ "CDC Fact Canvas – Chlamydia". Archived from the original on 16 Dec 2016. Retrieved 21 Baronial 2008.
- ^ "STD Trends in the The states: 2010 National Information for Gonorrhea, Chlamydia, and Syphilis". Centers for Disease Control and Prevention (CDC). 22 November 2010. Archived from the original on 24 January 2012.
- ^ "Untreatable gonorrhoea 'superbug' spreading around globe, WHO warns". The Daily Telegraph. 7 July 2017. Archived from the original on 7 July 2017.
- ^ "Daf Parashat Hashavua". Archived from the original on iii Oct 2012. Retrieved 2 Nov 2012.
- ^ Higgins, John (1587). The Mirror for Magistrates. equally cited in the Oxford English Dictionary entry for "clap"
- ^ Baarda, Benjamin I; Sikora, Aleksandra East (2015). "Proteomics of Neisseria gonorrhoeae: The treasure hunt for countermeasures against an old disease". Frontiers in Microbiology. 6: 1190. doi:10.3389/fmicb.2015.01190. PMC4620152. PMID 26579097.
- ^ Max Bough (1898). "Ueber neuere Antigonorrhoica (insbes. Argonin und Protargol)". Archives of Dermatological Enquiry. 43 (1): 31–36. doi:10.1007/BF01986890. S2CID 45492365.
- ^ MedlinePlus Encyclopedia: Neonatal Conjunctivitis
- ^ Westward Sanger. History of Prostitution. NY, Harper, 1910.
- ^ P. LaCroix. The History of Prostitution—Vol. two. NY, MacMillan, 1931.
- ^ a b Moen, Juliann (2017). Basic Healthcare Studies: Sexually Transmitted Disease. Lester Bivens. Alpha Editions. ISBN9789386367570.
- ^ Nosotros Leiky. History of European Morals. NY, MacMillan, 1926.
- ^ Jerse, AE; Fustigate, MC; Russell, MW (20 March 2014). "Vaccines confronting gonorrhea: current condition and future challenges". Vaccine. 32 (xiv): 1579–87. doi:ten.1016/j.vaccine.2013.08.067. PMC4682887. PMID 24016806.
- ^ Gottlieb, Sami Fifty.; Johnston, Christine (2017). "Future prospects for new vaccines against sexually transmitted infections". Curr Opin Infect Dis. xxx (1): 77–86. doi:x.1097/QCO.0000000000000343. PMC5325242. PMID 27922851.
- ^ Petousis-Harris, Helen (2017). "Effectiveness of a group B outer membrane vesicle meningococcal vaccine against gonorrhoea in New Zealand: a retrospective case-control written report". Lancet. 390 (10102): 1603–1610. doi:x.1016/S0140-6736(17)31449-6. PMID 28705462. S2CID 4230156.
External links
| | Wikimedia Commons has media related to Gonorrhea. |
- Gonorrhea at Curlie
- "Gonorrhea – CDC Fact Sheet"
Source: https://en.wikipedia.org/wiki/Gonorrhea
0 Response to "Gonorrhea Can Be Passed From the Mother to Her Baby"
Postar um comentário